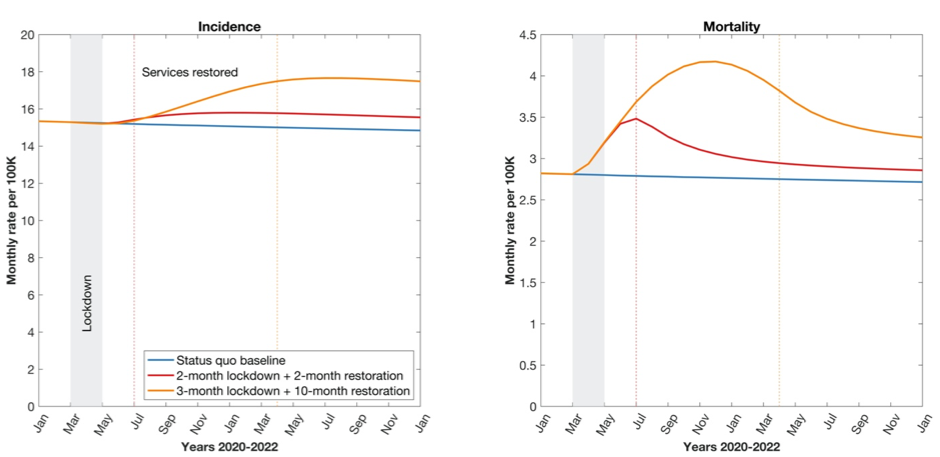
A new modelling report shows that a 3-month lockdown and a protracted 10-month restoration could lead to an additional 6.3 million cases of TB between 2020 and 2025, and an additional 1.4 million TB deaths during this time. The rates of TB incidence and death in 2021 will increase to levels last seen in 2013 and 2016 respectively.
Before the COVID-19 outbreak, we were eagerly awaiting the UN Secretary General’s report on progress that has been made against the targets in the landmark UN political declaration on TB in 2018, designed to accelerate progress on ending TB.
Big challenges remained, such as underfunding for TB programmes and TB research, issues with diagnosis leading to 30% of people with TB each year being “missed” and only 1 in 3 people with drug-resistant TB were enrolled on treatment.
But progress was being made. Organisations such as the Global Fund to Fight AIDS, TB and Malaria, the Stop TB Partnership and the World Health Organization were investing in approaches that worked, such as scaling up case finding.

The impact of COVID-19 on TB is due to a number of factors, including the impact of lockdowns on ability to access local health services. Other factors include, GeneXpert diagnostic machines are being repurposed for COVID-19 testing, personal protective equipment for health workers being used for COVID-19 leaving a shortage for TB workers, repurposing of national TB budgets, conversion of drug-resistant TB wards to COVID-19 wards, and disruptions to supply of essential TB medical commodities, including drugs.
Time and again, people with TB face a double burden during epidemics or pandemics. During the 2014-15 Ebola epidemic, Guinea saw a 53% decrease in the diagnosis rate of TB, and a doubling of the TB mortality. Countries around the world are following the same pattern during COVID-19 which high TB burden countries, such as India and South Africa reporting significant drops in diagnosis rates. 10-15 additional TB infections are transmitted per person with untreated TB per year. Mortality rates for untreated drug-susceptible and drug-resistant TB are 23% and 30% respectively.
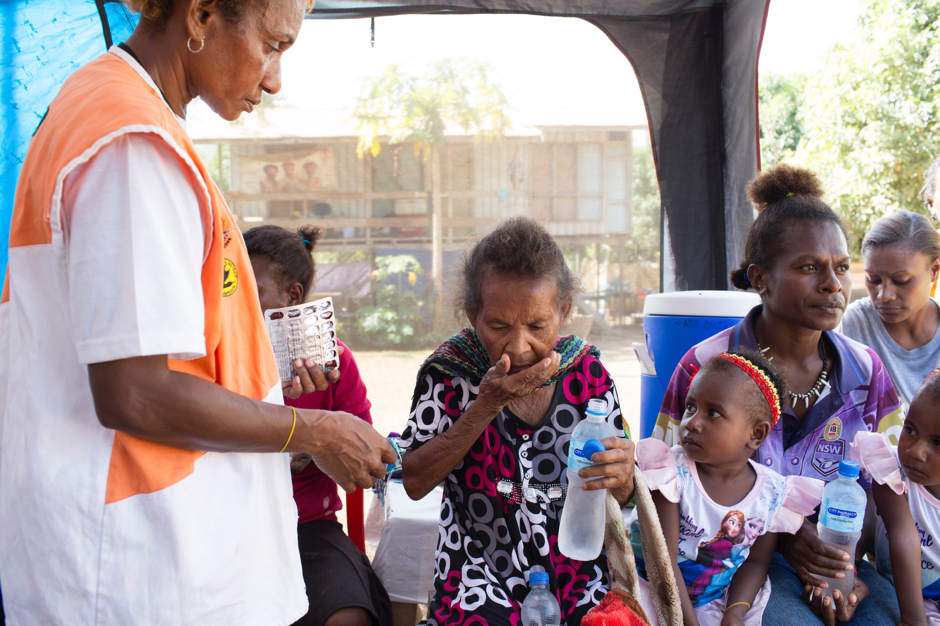
The progress made against TB must be regained through increased efforts and investments. This will include:
- Scaling up case finding, contact tracing, community engagement and use of new, innovative digital tools. This can take place alongside contact tracing and testing for COVID-19.
- Mitigating the impacts of interrupted supplies of quality assured, affordable treatment to prevent disruptions or delays to treatment.
- Ensuring that the development of new tools for TB is continued or expedited once possible.
- Protecting the most vulnerable people and ensuring that services reach everyone.
- Providing adequate protection for all health workers.
Weathering the COVID-19 storm will create short and long term impacts for TB. But it could also create opportunities, such as through increased capacity for contact tracing and testing, as well as widespread recognition of the need for adequate protection for health workers, for equitable research and development, and to protect and prioritise the most vulnerable.
