Since its creation, Global Fund has helped to save 27 million lives. Responsible for 65% of all international financing of the global TB response, its adequate financing will be a cornerstone of the success of the TB response for years to come.
5 reasons why it’s time to fully fund the Global Fund
1. It’s time for action

 Image: World Health Organisation
Image: World Health Organisation
In September 2018, world leaders attended the first UN High-Level Meeting on TB (HLM) and signed a political declaration. Commitments in the declaration include diagnosing and treating 40 million people with tuberculosis (TB) by 2022, fully financing the global response to TB including through mechanisms such as the Global Fund to Fight AIDS, TB and Malaria, closing the research and development (R&D) funding gap, and promoting and supporting an end to stigma and all forms of discrimination.
These promises, if delivered on, are transformative. But that is a big if. There have been countless commitments on paper but a significant lack of action. For example, world leaders committed to end TB by 2030 in the Sustainable Development Goals. But, at current rates of progress, this won’t be achieved for another 191 years.
The HLM commitments provide a roadmap for getting the world on track to end the world’s biggest infectious disease killer, and this year there is the first big test of each country’s resolve to deliver on it. The test is the replenishment of the Global Fund to Fight AIDS, TB and Malaria. Responsible for 65% of all international financing of the global TB response, its adequate financing will be a cornerstone of the success of the TB response for years to come. Since its creation, Global Fund has helped to save 27 million lives. It is a model that is proven to work and offers countries a cost-effective way of investing in global health, health systems strengthening, health security, sustainable development and universal health coverage (UHC).
2. It’s time for equity

Image: Tom Maguire.
Volunteer health worker Rodney Kove speaks to people with TB about the side effects of their treatment at an outreach post outside his home in ATS settlement, Port Moresby.
The Global Fund focuses on equity. This makes it a trailblazer in the era of sustainable development and in pursuit of UHC. Globally, about 40% of people with TB are never formally diagnosed every year. The reasons so many people are “missed” range from poor access to health services to unavailability of TB services in their local facility (especially at the primary care level) or a lack of health workers.
In Papua New Guinea, it is easy to see why this number is so high, where 85% of the population lives in a rural area and over 850 different languages are spoken, there is a deadly combination of inaccessibility to health services, low literacy rates and long and arduous treatment regimens, even in the capital, Port Moresby. Within a year, if a person has TB but is not diagnosed, they could pass it on to 15-20 other people. Therefore, it is essential to bring diagnosis and treatment to people, wherever they are, by people like Rodney Kove (pictured). This local action is a key facet of Global Fund’s work in saving lives.
In Papua New Guinea, the Global Fund operates its grant through NGOs, principally World Vision. One World Vision programme is the TB outreach post in ATS Settlement, where about 8,000 people live, including 74 people known to have TB. For those who are not yet diagnosed, the volunteers conduct community outreach and education to spread awareness of symptoms including through theatre, dispel myths rooted in sorcery, and guide people to where they can be diagnosed and treated. Providing treatment close to where people live is essential given that daily treatment is required and people cannot afford a daily bus fare.
Finding the “missing” people with TB is a key focus of Global Fund, therefore it plays a crucial role in delivering on the diagnosis and treatment targets of the HLM. Between 2018 and 2020, the Global Fund is giving specific attention to 13 countries that contribute about 75% of all “missing” people with TB globally. Collaborating with partners like WHO, Stop TB Partnership and the private sector to improve data systems, diagnosis and communication are some of the ways this can be done.
In India, collaboration with the private sector has been very successful and led to a sharp increase in the proportion of people with TB who are “found”

Image: Tom Maguire.
Rodney Kove’s house in ATS Settlement, Port Moresby.
3. It’s time for sustainability
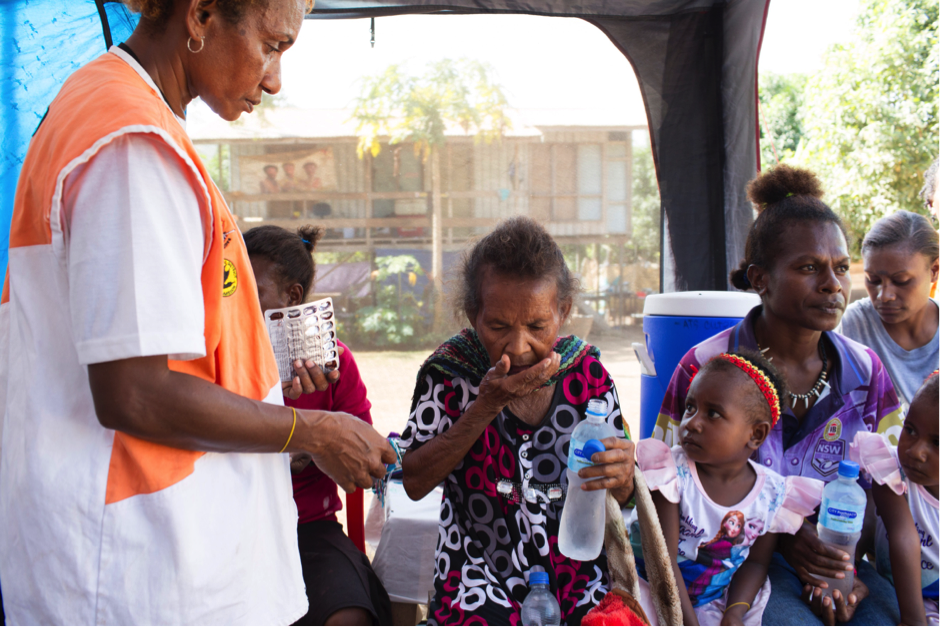
Image: Tom Maguire.
Twins Lynette and Anette watch as an elderly woman takes her TB medication, administered by volunteer Cathy Tolom. Lynette, like her mother, has TB and Annette is taking preventive therapy.
The Global Fund also focuses on health systems strengthening. 27% of Global Fund investments go to building resilient and sustainable systems for health. This could include improving data systems, procurement and supply chain management, commodity planning, logistics management, warehousing, information tracking. It includes integrated service delivery which focuses on each person.
Strong health systems are essential for global health security. This was tragically revealed during the height of the Ebola outbreak in West Africa 2014-15. Countries with stronger health systems such as Nigeria were able to contain the outbreak, while those with weaker systems such as Sierra Leone, Liberia and Guinea were unable to, leading to huge loss of life and knock-on impacts on the economy. It is thought the 2014-15 outbreak resulted in US$ 2.8 billion in economic losses. For HIV, TB and malaria drug-resistance poses a huge threat to global health security, and to the gains made against the three diseases so far. The Global Fund will play an instrumental role in containing and tackling the threat of drug-resistance.
Strengthening health systems also means bringing services closer to where people live. For example, the Ethiopian government has responded to the health care challenge of a primarily rural population by building or upgrading 15,000 village-level health care facilities, called health posts, across the country. As a result, more than 92% of Ethiopians live within 10 kilometres of a public health care facility. This has been supported by the Global Fund’s Health Service Extension Program, through which over 40,000 women have been trained to serve communities as health extension workers.
The consequences of unavailability of services at the nearest health facility are all too common in TB. For example, 5-month old Dulcie (pictured below), lost her mother to drug-resistant TB soon after she was born and contracted it herself. Her mother was too unwell to make the trip from their home in Kikori to the MSF hospital in Kerema, which was the only place she could receive the treatment she needed. Her local aid post did not provide drug-resistant TB treatment, but the MSF hospital is a 7-hour boat ride away, costing 300 kina (about £70). Dulcie’s auntie made the trip with her and they will both stay in Kerema until the treatment is complete.
TB is the only drug-resistant infection that is airborne and is responsible for one third of antimicrobial resistance-related deaths. Fewer than 20% of people with multi-drug resistant TB globally are correctly diagnosed and provided treatment. The Political Declaration of the UN High-Level Meeting on TB included a commitment to “provide diagnosis and treatment to 1.5 million people with drug-resistant TB from 2018-2022.” An adequately financed Global Fund will be essential for delivering on this.

Image: Tom Maguire
5 month old Dulcie (June 2018) contracted drug-resistant TB shortly after she was born. In this picture, she is 47 days into her treatment for drug-resistant TB and is being cared for her by aunt.
4. It’s time for innovation

Image: Tom Maguire.
Lab worker looks at sputum samples at 6 Mile Health Clinic, Port Moresby.
The Global Fund helps to increase access to the best tools to diagnose and treat TB, no matter how rural the setting. In India, the molecular diagnostic test, GeneXpert, that delivers rapid results including whether the strain of TB is drug resistant, is brought to health centres in a van. This enables more vulnerable people be reached with the best technology, even if their local health centre does not have the equipment or is out of reach entirely.
The Global Fund also promotes innovation in financing from other actors. For example, Global Fund’s multi-country grants for malaria have raised nearly twice as much in additional investment in the 2017-2019 period, including an expected US$100 million in domestic financing. This includes increased investment to tackle drug-resistant malaria, thereby increasing investment in global health security and fostering coordinated efforts between partners and countries. Multi-country grants help to expand access to malaria services, especially for underserved populations such as mobile and migrant populations.

Image: The Global Fund.
Blog: In Rural India, High-tech Vans Fund “Missing” TB Patients
5. Or else, we risk turning back time
The clock is ticking and the world is watching.

Image: Erick Okioma, Twitter